|
|||||||||
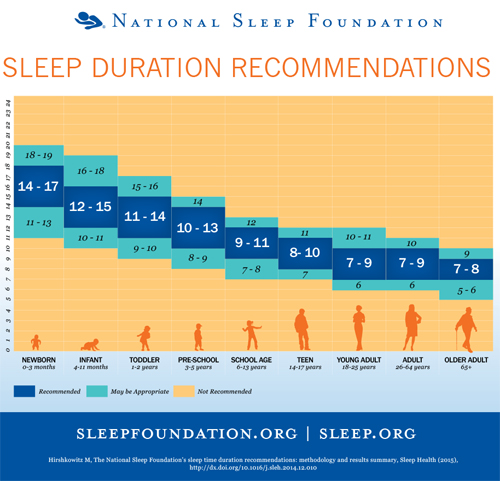
Getting Enough Sleep Is crucial for Good Health[1][2] Even though we know that lack of sleep makes us feel tired, sluggish, and irritable, most Americans don’t get enough. We and our children stay up too late watching television, to study, to work, to play, or to party and struggle to get out of bed when the alarm clock goes off in the morning. Many of us and our children have days when we, or they, or both of us are sleepy. Lack of sleep impairs attention, judgment, problem solving, ability to learn, thinking and mood. Lack of sleep is associated with poor school performance, weight gain, risk of diabetes and cardiovascular diseases. Lifelong healthy sleep habits are important to health. The glymphatic system to eliminate the brain’s waste products such as the beta-amyloid associated with Alzheimer’s dementia functions mainly during sleep.[3] Furthermore, there is evidence that untreated sleep apnea (transient periods when breathing stops), a cause of disrupted sleep, is associated with mild cognitive impairment and Alzheimer’s disease 10 years sooner than its occurrence among those without the disorder.[4] Although it is not possible to definitively say if poor sleep is the cause or the result of the brain microinfarcts that are linked to dementia, there is a strong association between sleep disturbance and dementia. In one study researchers found that after they died, the one-quarter of men with the lowest oxygen levels during prior sleep tests were almost four times more likely to show microinfarcts in the brain, compared to men with the highest oxygen levels. Men who spent less time in slow-wave sleep — the deep, restorative stage of sleep — tended to show more atrophy in their brain tissue.[5] In the process of learning something new, there is good evidence for the theory that sleep helps to establish a stable memory and the ability to recall the information. Conversely, with a sleep deficit, memory and many other aspects of cognitive functioning are impaired and we may become dangerous—for example prone to schoolyard accidents, and crashes while driving. Investigators believe that slowed thinking and impaired decision making from sleep deprivation was a significant factor in many well-known disasters including the 1979 nuclear accident at Three Mile Island, the 1986 nuclear meltdown at Chernobyl, the grounding of the Exxon Valdez oil tanker, and the explosion of the space shuttle Challenger. [6] [7]A National Sleep Foundation survey found that sixty percent of adult drivers have driven a vehicle when drowsy and more than one-third have fallen asleep at the wheel. The Division of Sleep Medicine at the Harvard Medical School reports that “The Institute of Medicine estimates—based on recent high quality naturalistic and epidemiologic studies—that drowsy driving is responsible for fully 20 percent of all motor vehicle crashes. That would mean that drowsy driving causes approximately 1 million crashes, 500,000 injuries, and 8,000 deaths each year in the U.S.” The National Sleep Foundation convened a panel of experts to consider how to avoid drowsy driving. They agreed upon the following expert consensus statement: “Drivers who have slept for two hours or less in the preceding 24 hours are not fit to operate a motor vehicle.” Panelists further agreed that most healthy drivers would likely be impaired if they got only 3 to 5 hours of sleep during the prior 24 hours. [8] Research on the function and benefits of sleep reveal it has an important role in repair and restoration of muscles, the brain and many vital bodily functions including maintenance of a healthy balance of hormones, regulating hunger, supporting the immune system, and facilitating memory and learning. Chronic sleep deprivation is associated with an increased risk of mental distress and major illnesses, obesity, diabetes, high blood pressure and cardiovascular disease including stroke. Epidemiological studies have found that sleeping five hours or less per night is associated with an increased all-cause mortality risk of about 15 percent. [9] [10] [11] [12] [13] Many children and teens are going to bed too late to get an optimal night’s rest. Research shows that children who go to bed after 9:00 p.m. take longer to fall asleep, wake more often at night and get less overall sleep. Parents should be aware of how much sleep their child needs and establish an appropriate bedtime. More than a third of American adults are not getting enough sleep on a regular basis, according to a 2016 Centers for Disease Control and Prevention (CDC) study.[14] In one study more than 40% of children had at least one sleep related health problem such as sleep-disordered breathing, insomnia (trouble falling or staying asleep), and excessive sleepiness. Some children have symptoms such as sleep terrors, sleepwalking, or nocturnal bruxism (teeth grinding). [15] Between 25% and 50% of parents of children with ADHD (attention deficit hyperactivity disorder) have sleep problems such as difficulty with initiating and maintaining sleep. [16] Circadian rhythms are the biological clock that regulates the timing of periods of sleepiness and wakefulness throughout the day. They are established by exposure to light and darkness. In newborns, the rhythms begin to develop at about six weeks, and by three to six months most infants have a regular sleep-wake cycle. Sleep is especially important for children as it directly impacts mental and physical development. At puberty, the circadian rhythms that once made a child sleepy around 8:00 or 9:00 pm begin to shift. The feeling of a desire to sleep is delayed for about two hours to around 10:00 or 11:00 pm. Because most teens have to wake up early for school, it is important for them to go to bed on time so they can get between 8 and 10 hours of sleep––but one study found that only 15% of teens reported sleeping 8 1/2 hours on school nights. It is important for teens to resist the temptation to stay up too late at night doing homework, playing games, texting or talking with friends. Even worse for healthy sleep, they may stay out too late, drink, smoke, or use drugs. Many teens fight a daily battle against sleepiness, struggle to wake up and make it to school on time and are grouchy and irritable. Over time, nights of too little sleep can build into a sleep deficit. Tired and sleepy teens are more likely to underperform in school, sports, or at work. Back to topAddressing Sleep Problems Excessive daytime sleepiness or suddenly falling asleep on the job or while driving is dangerous and not normal. It can be the sign of a medical condition that requires treatment. These conditions include obstructive sleep apnea (OSA), periodic limb movements of sleep (PLMS) and restless legs syndrome (RLS), sleepwalking and narcolepsy, a brain disorder causing sudden attacks of falling asleep. Teens and adults with periodic limb movement disorder (PLMD) or restless legs syndrome (RLS) find their sleep is disrupted by leg (or, less commonly, arm) movements, leaving them tired or irritable from lack of sleep. Obstructive Sleep Apnea (OSA) is under diagnosed but common in the U.S. with 34% of men and 17% of women affected. [19] It occurs when a person’s airway becomes partially or completely blocked many times during a night of sleep, leading to decreased airflow or short-term cessation of breathing, repetitive awakenings and severely disrupted sleep. Medical care for individuals with OSA is indicated because it causes episodes of oxygen deprivation that can lead to high blood pressure, insulin resistance, heart disease, mood and memory problems.[20] Obesity is the greatest risk factor for OSA and weight loss may ease its severity or eliminate it. Teens with obstructive sleep apnea might snore, have difficulty breathing, and even sweat heavily during sleep. Because it disrupts sleep, they may feel extremely sleepy or irritable during the day. Teens with sleep apnea or indicative symptoms (such as loud snoring or excessive daytime sleepiness) should be checked by a doctor. Treatments may be necessary including use of a continuous positive airway pressure machine, optimizing sleep position, sleeping with dental devices that reposition the lower jaw, and surgical procedures that widen the airway. Other treatments that may help sleep disorders include cognitive behavioral therapy, meditation and biofeedback to ease stress and prescription medications.[21] Over-the-counter sleep medications and remedies, including a low dose of melatonin, may help some people. Melatonin supplements the body’s natural production of the sleep inducing hormone but it may have side-effects, like headache, dizziness, day time grogginess and interfere with blood pressure medications. The long-term effects and safety for adults and children are not known. Be aware that melatonin can be sold as a dietary supplement so quality may be poorly regulated. Only obtain melatonin in a pharmaceutical grade from a reputable source. Herbal sleep remedies have not been proven to be effective. Prescribed drugs have the problem of inhibiting natural sleep, drowsiness the following day and possibly serious mental and physical problems. The optimal duration of sleep varies between individuals. Although some people think they do fine on five or six hours a night, the optimal sleep duration for most people is between seven and eight hours a night. The chart below provides recommendations from the National Sleep Foundation.[22] [23]
For the average American of all ages, the most likely reason for lack of sleep is because we do not set aside enough time for it. We stay up too late and are groggy when the alarm goes off the next morning. In addition to planning for enough time for sleep, the Division of Sleep Medicine at the Harvard Medical School offers this advice for getting the rest you need:[24]
Back to top [1] Healthy Sleep. Division of Sleep Medicine. Harvard Medical School. http://healthysleep.med.harvard.edu/healthy/.
[2]The ABCs of sleep. University of California Wellness Letter. 30:2, Fall 2013.
[3]Nedergaard M, Goldman SA. The Brain's Waste-Disposal System May Be Enlisted to Treat Alzheimer's and Other Brain Illnesses. Scientific American. March 2016.
[4]Osorio RS, Gumb T, Pirraglia E. et al. Sleep-disordered breathing advances cognitive decline in the elderly Neurology-2015:84;1964-71.
[5]Rebecca P. Gelber RP, Susan Redline S, Ross GW et al. Associations of brain lesions at autopsy with polysomnography features before death. Neurology 2014 : WNL.0000000000001163v1-10.1212/WNL.0000000000001163.
[6]Healthy Sleep. Division of Sleep Medicine. Harvard Medical School. http://healthysleep.med.harvard.edu/healthy/
[7]Sigurdson K, Ayas N. The public health and safety consequences of sleep disorders. Canadian J Physiol Pharmacol. 2007; 85:179-183.
[9]Healthy Sleep. Division of Sleep Medicine. Harvard Medical School. http://healthysleep.med.harvard.edu/healthy/
[10]Sigurdson K, Ayas N. The public health and safety consequences of sleep disorders. Canadian J Physiol Pharmacol. 2007; 85:179-183.
[11]Hublin C, Partinen M, Koskenvuo M, Kaprio J. Sleep and mortality: a population-based 22-year follow-up study. Sleep. 2007; 30(10):1245-53.
[12]Patel SR, Ayas NT, Malhotra MR, White DP, Schernhammer ES, Speizer FE, Stampfer MJ, Hu FB. A prospective study of sleep duration and mortality risk in women. Sleep. 2004; 27(3):440-4.
[13]Gallicchio L, Kalesan B. Sleep duration and mortality: a systematic review and meta-analysis. J Sleep Res 2009; 18:148–58.
[14]Liu Y, Wheaton AG, Chapman DP, Cunningham TJ, Lu H, Croft JB. Prevalence of Healthy Sleep Duration among Adults — United States, 2014. MMWR Morb Mortal Wkly Rep 2016;65:137–141. DOI: http://dx.doi.org/10.15585/mmwr.mm6506a1.
[15]Archbold KH, et al. Symptoms of sleep disturbances among children at two general pediatric clinics. J Pediatr. 2002;140(1):97–102.
[16]Spruyt K, Gozal D. Sleep disturbances in children with attention-deficit/hyperactivity disorder. Expert review of neurotherapeutics. 2011;11(4):565-577. doi:10.1586/ern.11.7.
[17] Healthy Sleep. Division of Sleep Medicine. Harvard Medical School. http://healthysleep.med.harvard.edu/healthy/.
[18]Healthy Sleep. Division of Sleep Medicine. Harvard Medical School. http://healthysleep.med.harvard.edu/healthy/
[19]Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM. Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol. 2013;177(9):1006-1014.
[20]
Redline S. Screening for Obstructive Sleep Apnea Implications for the Sleep Health of the Population. JAMA.2017;317(4):368-370. doi:10.1001/jama.2016.18630.
[21] Medalie L, Cifu AS. Management of Chronic Insomnia Disorder in Adults. JAMA. 2017;317(7):762-763. doi:10.1001/jama.2016.19004
[23] Watson NF, Badr MS, Belenky G, et al. ; Consensus Conference Panel. Joint consensus statement of the American Academy of Sleep Medicine and Sleep Research Society on the recommended amount of sleep for a healthy adult: methodology and discussion. Sleep 2015;38:1161–83.
[24]Healthy Sleep. Division of Sleep Medicine. Harvard Medical School. http://healthysleep.med.harvard.edu/healthy/
|
|
|||